Introduction
Folate transport disorders in children affect the brain’s ability to receive and use folate, a nutrient essential for neurological development, learning, behavior, and long-term cognitive health. When folate cannot reach the central nervous system in adequate amounts, children may experience developmental delays, behavioral changes, motor challenges, or other neurological symptoms that can progress without proper support. Understanding the core facts about these disorders helps families navigate testing, treatment, and supportive care with greater clarity. The following sections outline key information that can guide more informed conversations with practitioners and help identify pathways that are often overlooked in standard clinical training.
Folate Transport Disorders Involve Disrupted Movement of Folate Into the Brain
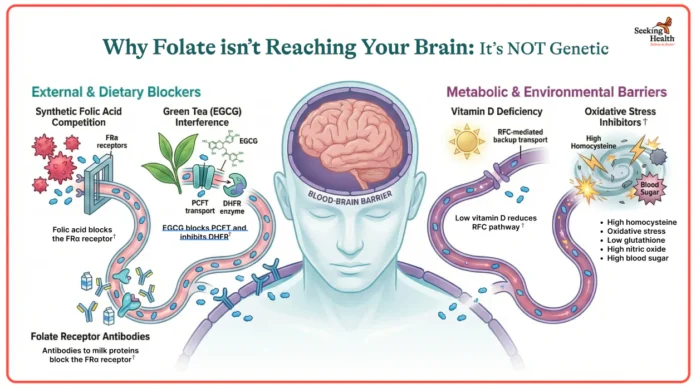
Folate transport disorders occur when the body cannot move folate efficiently across the blood brain barrier. This may happen due to genetic variations, autoantibodies that block folate receptors, or metabolic challenges that interfere with folate utilization. When folate cannot enter the brain, neurological function becomes compromised even if blood folate levels appear normal. This distinction is important because many families are told that folate status is adequate based on standard blood tests, yet the brain may still be deficient. Discussing specialized testing with a practitioner, including folate receptor antibody testing or cerebrospinal fluid folate evaluation, can help uncover issues that routine assessments may miss. These tests are not always part of standard training, which is why families often need to request them specifically.
Treatment Often Requires Specialized Folate Forms That Bypass Transport Barriers
Once a folate transport disorder is identified, treatment typically focuses on providing forms of folate that can reach the brain more effectively. Some children respond well to targeted folate formulations that support neurological pathways even when transport is impaired. A video that will explain why this is especially relevant for families exploring the connection between Cerebral Folate Deficiency and Autism, as some children benefit from therapies that address underlying metabolic and transport challenges. Many clinicians share educational resources, including a video that will explain why Cerebral Folate Deficiency and Autism is an important topic for families seeking clarity about treatment options. These therapies are often introduced gradually and monitored closely to ensure the child is responding well. Because these approaches are not always emphasized in traditional medical training, families may need to initiate conversations about specialized folate support and individualized dosing strategies.
Nutrition and Metabolic Support Can Strengthen Treatment Outcomes
Although medical therapy is central to addressing folate transport disorders, nutrition plays a meaningful role in supporting the body’s ability to use folate effectively. Children may benefit from diets rich in natural folate sources, antioxidants, and nutrients that support mitochondrial function. Some practitioners also explore metabolic testing to identify nutrient deficiencies or imbalances that may influence folate pathways. These assessments can reveal patterns that standard evaluations overlook, such as low levels of cofactors needed for folate metabolism or signs of oxidative stress that may interfere with neurological function. Discussing these nutritional and metabolic considerations with a practitioner can help create a more comprehensive treatment plan that supports the child’s overall health and developmental progress.
Early Identification and Ongoing Monitoring Improve Long Term Outcomes
Early recognition of folate transport disorders allows children to receive support during critical periods of brain development. Once treatment begins, ongoing monitoring helps practitioners adjust therapy based on the child’s growth, symptoms, and neurological changes. Families may notice improvements in communication, behavior, motor skills, or cognitive function over time, although progress varies from child to child. Regular follow up also ensures that nutritional strategies, metabolic support, and folate therapy remain aligned with the child’s evolving needs. Because many aspects of folate transport disorders fall outside standard pediatric training, families often benefit from working with practitioners who are familiar with metabolic medicine, functional nutrition, or neurodevelopmental specialties. These professionals can help guide testing, interpret results, and recommend supportive pathways that may not be included in conventional care models.
Collaborative Care Helps Families Navigate Complex Needs
Folate transport disorders often require a collaborative approach that includes medical treatment, nutritional guidance, developmental support, and ongoing evaluation. Families may work with pediatricians, neurologists, dietitians, therapists, and specialists who understand the nuances of folate metabolism. This team based approach helps ensure that the child receives comprehensive care that addresses both the biological and developmental aspects of the condition. Parents are encouraged to discuss all potential support pathways with their practitioner, including testing options, nutritional strategies, and therapeutic interventions that may not be routinely offered. When families are informed and proactive, they can help shape a care plan that supports their child’s long-term neurological health.
Conclusion
Folate transport disorders in children require thoughtful evaluation, targeted treatment, and supportive care that extends beyond standard clinical practices. By understanding how these disorders affect the brain, exploring specialized testing, considering nutritional and metabolic support, and working closely with knowledgeable practitioners, families can create a more complete pathway toward improved neurological function and developmental progress.